Within the early 2010s, electrical energy appeared poised for a hostile takeover of your physician’s workplace. Analysis into how the nervous system controls the immune response was gaining traction. And that had opened the door to the opportunity of hacking into the physique’s circuitry and thereby controlling a number of power ailments, together with rheumatoid arthritis, bronchial asthma, and diabetes, as if the immune system had been as reprogrammable as a pc.
To do this you’d want a brand new class of implant: an “electroceutical,” formally launched in an article in Nature in 2013. “What we’re doing is growing gadgets to exchange medication,” coauthor and neurosurgeon Kevin Tracey advised Wired UK. These would grow to be a “mainstay of medical remedy.” No extra messy unwanted side effects. And no extra guessing whether or not a drug would work otherwise for you and another person.
There was cash behind this imaginative and prescient: the British pharmaceutical big GlaxoSmithKline introduced a $1 million analysis prize, a $50 million enterprise fund, and an formidable program to fund 40 researchers who would determine neural pathways that might management particular ailments. And the corporate had an aggressive timeline in thoughts. As one GlaxoSmithKline govt put it, the objective was to have “the primary drugs that speaks {the electrical} language of our physique prepared for approval by the top of this decade.”
Within the 10 years or so since, round a billion {dollars} has accreted across the effort by means of direct and oblique funding. Some implants developed in that electroceutical push have trickled into scientific trials, and two corporations affiliated with GlaxoSmithKline and Tracey are ramping up for splashy bulletins later this 12 months. We don’t know a lot but about how profitable the trials now underway have been. However widespread regulatory approval of the kinds of gadgets envisioned in 2013—gadgets that could possibly be utilized to a broad vary of power ailments—will not be imminent. Electroceuticals are a good distance from fomenting a revolution in medical care.
On the similar time, a brand new space of science has begun to cohere round one other means of utilizing electrical energy to intervene within the physique. As a substitute of focusing solely on the nervous system—the freeway that carries electrical messages between the mind and the physique—a rising variety of researchers are discovering intelligent methods to electrically manipulate cells elsewhere within the physique, comparable to pores and skin and kidney cells, extra immediately than ever earlier than. Their work means that this strategy might match the early promise of electroceuticals, yielding fast-healing bioelectric bandages, novel approaches to treating autoimmune issues, new methods of repairing nerve injury, and even higher remedies for most cancers. Nevertheless, such ventures haven’t benefited from funding largesse. Traders have a tendency to know the connection between biology and electrical energy solely within the context of the nervous system. “These assumptions come from biases and blind spots that had been baked in throughout 100 years of neuroscience,” says Michael Levin, a bioelectricity researcher at Tufts College.
Electrical implants have already had success in focusing on particular issues like epilepsy, sleep apnea, and catastrophic bowel dysfunction. However the broader imaginative and prescient of changing medication with nerve-zapping gadgets, particularly ones that alter the immune system, has been slower to materialize. In some instances, maybe the nervous system will not be one of the best ways in. Trying past this singular locus of management may open the best way for a wider suite of electromedical interventions—particularly if the nervous system proves much less amenable to hacking than initially marketed.
The way it began
GSK’s formidable electroceutical enterprise was a response to an more and more onerous drawback: 90% of medicine fall down through the impediment race by scientific trials. A brand new drug that does squeak by can value $2 billion or $three billion and take 10 to 15 years to convey to market, a galling return on funding. The flaw is within the supply system. The best way we administer therapeutic chemical compounds hasn’t had a lot of a conceptual overhaul because the Renaissance doctor Paracelsus: ingest or inject. Each approaches have built-in inefficiencies: it takes a very long time for the medication to construct up in your system, and so they can disperse extensively earlier than arriving in diluted type at their goal, which can make them ineffective the place they’re wanted and poisonous elsewhere. Tracey and Kristoffer Famm, a coauthor on the Nature article who was then a VP at GlaxoSmithKline, defined on the publicity circuit that electroceuticals would remedy these issues—appearing extra shortly and dealing solely within the exact spot the place the intervention was wanted. After 500 years, lastly, right here was a brand new concept.
Nicely … new-ish. Electrically stimulating the nervous system had racked up promising successes because the mid-20th century. For instance, the signs of Parkinson’s illness had been handled by way of deep mind stimulation, and intractable ache by way of spinal stimulation. Nevertheless, these interventions couldn’t be undertaken calmly; the implants wanted to be positioned within the backbone or the mind, a frightening prospect to entertain. In different phrases, this concept would by no means be a cash spinner.
What acquired GSK excited was current proof that well being could possibly be extra broadly managed, and by nerves that had been simpler to entry. By the daybreak of the 21st century it had grow to be clear you can faucet the nervous system in a means that carried fewer dangers and extra rewards. That was due to findings suggesting that the peripheral nervous system—primarily, every part however the mind and backbone—had a lot wider affect than beforehand believed.
The prevailing knowledge had lengthy been that the peripheral nervous system had just one job: sensory consciousness of the skin world. This info is ferried to the mind alongside many little neural tributaries that emerge from the extremities and organs, most of which converge right into a single essential avenue on the torso: the vagus nerve.
Beginning within the 1990s, analysis by Linda Watkins, a neuroscientist main a workforce on the College of Colorado, Boulder, advised that this essential superhighway of the peripheral nervous system was not a one-way road in any case. As a substitute it appeared to hold message site visitors in each instructions, not simply into the mind however from the mind again into all these organs. Moreover, it appeared that this comms hyperlink permits the mind to exert some management over the immune system—for instance, stoking a fever in response to an an infection.
And in contrast to the mind or spinal wire, the vagus nerve is relatively straightforward to entry: its path to and from the mind stem runs near the floor of the neck, alongside an enormous cable on both aspect. You can simply pop an electrode on it—usually on the left department—and get zapping.
Meddling with the circulate of site visitors up the vagus nerve on this means had efficiently handled points within the mind, particularly epilepsy and treatment-resistant despair (and electrical implants for these purposes had been accepted by the FDA across the flip of the millennium). However the insights from Watkins’s workforce put the down path in play.
It was Kevin Tracey who joined all these dots, after which it didn’t take lengthy for him to grow to be the general public face of analysis on vagus nerve stimulation. Through the 2000s, he confirmed that electrically stimulating the nerve calmed irritation in animals. This “inflammatory reflex,” as he got here to name it, implied that the vagus nerve might act as a change able to turning off a variety of ailments, primarily hacking the immune system. In 2007, whereas based mostly at what’s now referred to as the Feinstein Institute for Medical Analysis, in New York, he spun his insights off right into a Boston startup referred to as SetPoint Medical. Its intention was to develop gadgets to flip this change and produce aid, beginning with inflammatory bowel illness and rheumatoid arthritis.
By 2012, a coordinated relationship had developed between GSK, Tracey, and US authorities companies. Tracey says that Famm and others contacted him “to assist them on that Nature article.” A 12 months later the electroceuticals street map was able to be introduced to the general public.
The story the researchers advised concerning the future was elegant and easy. It was illustrated by a story Tracey recounted steadily on the publicity circuit, of a first-in-human case research SetPoint had coordinated on the College of Amsterdam’s Educational Medical Heart. That workforce had implanted a vagus nerve stimulator in a person affected by rheumatoid arthritis. The stimulation triggered his spleen to launch a chemical referred to as acetylcholine. This in flip advised the cells within the spleen to modify off manufacturing of inflammatory molecules referred to as cytokines. For this man, the strategy labored nicely sufficient to let him resume his job, play along with his children, and even take up his outdated hobbies. Actually, his overenthusiastic resumption of his former actions resulted in a sports activities damage, as Tracey delighted in recounting for reporters and conferences.
Such case research opened the cash spigot. The mix of a wider vary of illness targets and fewer dangerous surgical targets was an investor’s love language. The place deep mind stimulation and different invasive implants had been restricted to uncommon, obscure, and catastrophic issues, this new interface with the physique promised many extra prospects: the power ailments now on the desk are way more prevalent, together with not solely rheumatoid arthritis however diabetes, bronchial asthma, irritable bowel syndrome, lupus, and lots of different autoimmune issues. GSK launched an funding arm it dubbed Motion Potential Enterprise Capital Restricted, with $50 million within the coffers to put money into the applied sciences and firms that may flip the futuristic imaginative and prescient of electroceuticals into actuality. Its inaugural funding was a $5 million stake in SetPoint.
Should you had been superstitious, what occurred subsequent may need regarded like an omen. The phrase “electroceutical” already belonged to another person—an organization referred to as Ivivi Applied sciences had trademarked it in 2008. “I’m pretty sure we despatched them a letter quickly after they began that marketing campaign, to alert them of our trademark,” says Sean Hagberg, a cofounder after which chief science officer on the firm. Right now neither GSK nor SetPoint can formally name its tech “electroceuticals,” and each check with the implants they’re growing as “bioelectronic drugs.” Nevertheless, this umbrella time period encompasses a variety of different interventions, some fairly nicely established, together with mind implants, backbone implants, hypoglossal nerve stimulation for sleep apnea (which targets a motor nerve operating by the vagus), and different peripheral-nervous-system implants, together with these for folks with extreme gastric issues.

The following drawback appeared briefly order: easy methods to goal the proper nerve. The vagus nerve has roughly 100,000 fibers packed tightly inside it, says Kip Ludwig, who was then with the US Nationwide Institutes of Well being and now co-directs the Wisconsin Institute for Translational Neuroengineering on the College of Wisconsin, Madison. These myriad fibers hook up with many alternative organs, together with the larynx and decrease airways, and electrical fields will not be exact sufficient to hit a single one with out hitting a lot of its neighbors (as Ludwig places it, “electrical fields [are] actually promiscuous”).
This explains why a wholesale zap of all the bundle had lengthy been related to unpredictable “on-target results” and unsightly “off-target results,” which is one other means of claiming it didn’t at all times work and will carry unwanted side effects that ranged from the irritating, like a power cough, to the life-altering, together with complications and a shortness of breath that’s higher described as air starvation. Singling out the fibers that led to the actual organ you had been after was arduous for one more cause, too: the present maps of the human peripheral nervous system had been outdated and fairly restricted. Such a low-resolution street map wouldn’t be ample to get a sign from the freeway all the best way to a vacation spot.
In 2014, to treatment this and usually advance the sphere of peripheral nerve stimulation, the NIH introduced a analysis initiative generally known as SPARC—Stimulating Peripheral Exercise to Relieve Circumstances—with the intention of pouring $248 million into analysis on new methods to use the nervous system’s electrical pathways for drugs. “My job,” says Gene Civillico, who managed this system till 2021, “was to do a program associated to electroceuticals that used the NIH coverage choices that had been obtainable to us to attempt to make one thing catalytic occur.” The thought was to make neural anatomical maps and type out the implications of following numerous paths. After the organs had been mapped, Civillico says, the subsequent step was to determine which nerve circuit would stimulate them, and decide on an entry level—“And the entry level must be the vagus nerve, as a result of that’s the place probably the most curiosity is.”
Two years later, as SPARC started to distribute its funds, corporations moved ahead with plans for the primary era of implants. GSK teamed up with Verily (previously Google Life Sciences) on a $715 million analysis initiative they referred to as Galvani Bioelectronics, with Famm at its helm as president. SetPoint, which had relocated to Valencia, California, moved to an expanded location, a campus that had as soon as housed a secret Lockheed R&D facility.
The way it’s going
Ten years after electroceuticals entered (after which shortly departed) the lexicon, the SPARC program has yielded essential details about {the electrical} particulars of the peripheral nervous system. Its maps have illuminated nodes which are each surgically engaging and medically related. It has funded a world constellation of educational researchers. However its insights will probably be helpful for the subsequent era of implants, not these in trials immediately.
Right now’s implants, from SetPoint and Galvani, will probably be within the information later this 12 months. Although SetPoint estimates that an prolonged research of its part III scientific trial will conclude in 2027, the first outcomes will probably be launched this summer season, says Ankit Shah, a advertising VP at SetPoint. And whereas Galvani’s trial will conclude in 2029, Famm says, the corporate is “coming to an thrilling level” and can publish affected person knowledge later in 2024.
The outcomes could possibly be interpreted as a referendum on the 2 corporations’ totally different approaches. Each gadgets deal with rheumatoid arthritis, and each goal the immune system by way of the peripheral nervous system, however that’s the place the similarities finish. SetPoint’s gadget makes use of a clamshell design that cuffs across the vagus nerve on the neck. It stimulates for only one minute, as soon as per day. SetPoint representatives say they’ve by no means seen the kinds of unwanted side effects which have resulted from utilizing such stimulators to deal with epilepsy. But when anybody did expertise these described by different researchers—even vomiting and complications—they is likely to be tolerable in the event that they solely lasted a minute.
However why not keep away from the vagus nerve fully? Galvani is utilizing a extra exact implant that targets the “finish organ” of the spleen. If the vagus nerve could be thought-about the primary freeway of the peripheral nervous system, an finish organ is actually a specific organ’s “driveway.” Galvani’s goal is the purpose the place the splenic nerve (having cut up off from a system linked to the vagus freeway) meets the spleen.
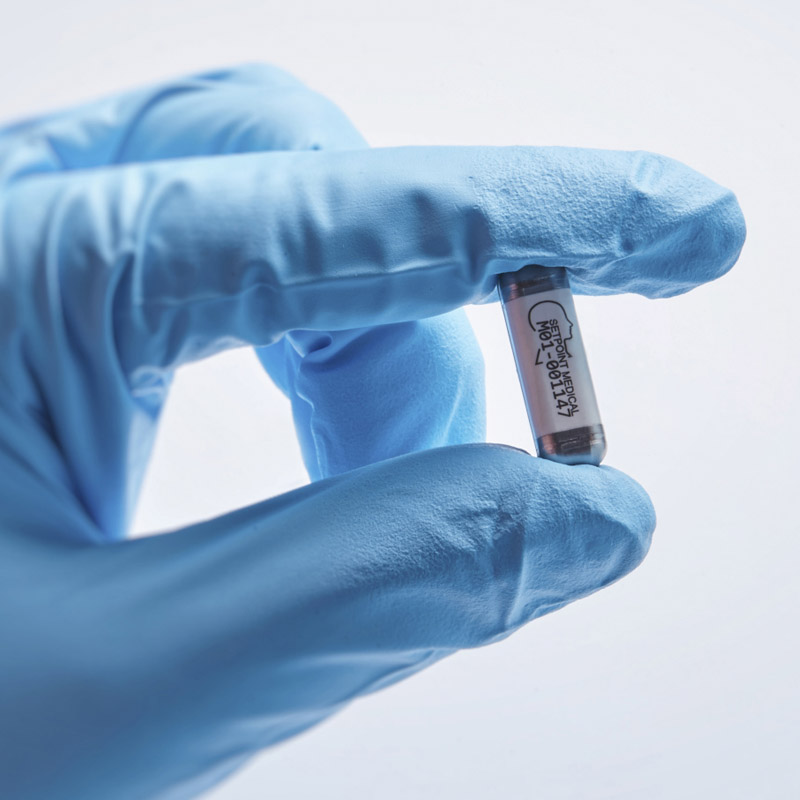
To zero in on such a particular goal, the corporate has sacrificed ease of entry. Its implant, which is concerning the dimension of a home key, is laparoscopically injected into the physique by the stomach button. Famm says if this strategy works for rheumatoid arthritis, then it can seemingly translate for all autoimmune issues. Highlighting this scientific trial in 2022, he advised Nature Opinions: “That is what makes the subsequent 10 years thrilling.”

Maybe extra so for researchers than for sufferers, nonetheless. At the same time as Galvani and SetPoint put together speaking factors, different SPARC-funded teams are nonetheless pondering the kinds of analysis questions suggesting that one of the best technological interface with the immune system continues to be up for debate. In the mean time, electroceuticals are within the highlight, however they’ve an extended technique to go, says Vaughan Macefield, a neurophysiologist at Monash College in Australia, whose work is funded by a newer $21 million SPARC grant: “It’s a sublime concept, [but] there are conflicting views.”
Macefield doesn’t suppose zapping all the bundle is a good suggestion. Many researchers are engaged on methods to get extra selective about which explicit fibers of the vagus nerve they stimulate. Some are designing novel electrodes that may penetrate particular fibers relatively than clamping round all of them. Others try to hit the vagus at deeper factors within the stomach. Certainly, some aren’t positive both electrical energy or an implant is a vital ingredient of the “electroceutical.” As a substitute, they’re pivoting from electrical stimulation to ultrasound.
The sheer vary of those approaches makes it fairly clear that the electroceutical’s remaining type continues to be an open analysis query. Macefield says we nonetheless don’t know the nitty-gritty of how vagus nerve stimulation works.
Nevertheless, Tracey thinks the number of approaches being developed doesn’t contravene the deserves of the essential concept. How tech corporations will make this work within the clinic, he says, is a separate enterprise and IP query: “Are you able to do it with centered ultrasound? Are you able to do it with a tool implanted with stomach surgical procedure? Are you able to do it with a tool implanted within the neck? Are you able to do it with a tool implanted within the mind, even? All of those methods are enabled by the concept of the inflammatory reflex.” Till scientific trial knowledge is in, he says, there’s no level arguing about one of the best ways to govern the mechanism—and if one strategy fails to work, that isn’t a referendum on the validity of the inflammatory reflex.
After stepping down from SetPoint’s board to renew a purely consulting position in 2011, Tracey centered on his lab work on the Feinstein Institute, which he directs, to deepen understanding of this pathway. The analysis there’s wide-ranging. A number of researchers beneath his remit are exploring a sort of noninvasive, oblique manipulation referred to as transcutaneous auricular vagus nerve stimulation, which stimulates the pores and skin of the ear with a wearable gadget. Tracey says it’s a “malapropism” to name this strategy vagus nerve stimulation. “It’s simply an ear buzzer,” he says. It might stimulate a sensory department of the vagus nerve, which can interact the inflammatory reflex. “However no one is aware of,” he says. Nonetheless, a number of scientific trials are underway.
“These items take time,” Tracey says. “This can be very troublesome to invent and develop a very revolutionary new factor in drugs. Within the historical past of drugs, something that was really new and revolutionary takes between 20 and 40 years from the time it’s invented to the time it’s extensively adopted.”
“Because the discoverer of this pathway,” he says, “what I wish to see is a number of therapies, serving to hundreds of thousands of individuals.” This imaginative and prescient will hinge on larger trials carried out over many extra years. These are usually about as arduous for gadgets as they’re for medication. Many outcomes that look compelling in early trials disappoint in later rounds—simply as for medication. It is going to be doable, says Ludwig, “for them to move a short-duration FDA trial but nonetheless actually not be a serious enchancment over the drug options.” Even after FDA approval, ought to it come, but extra research will probably be wanted to find out whether or not the implants are topic to the identical points that plague medication, together with habituation.
This imaginative and prescient of electroceuticals appears to have positioned a few billion eggs into the one basket of the peripheral nervous system. In some methods, this is smart. In any case, the obtained knowledge has it that these nervous alerts are the one technique to exert electrical management of the opposite cells within the physique. These different trillions—the pores and skin cells, the immune cells, the stem cells—are past the attain of direct electrical intervention.
Besides previously 20 years it’s grow to be abundantly clear that they aren’t.
Different cells converse electrical energy
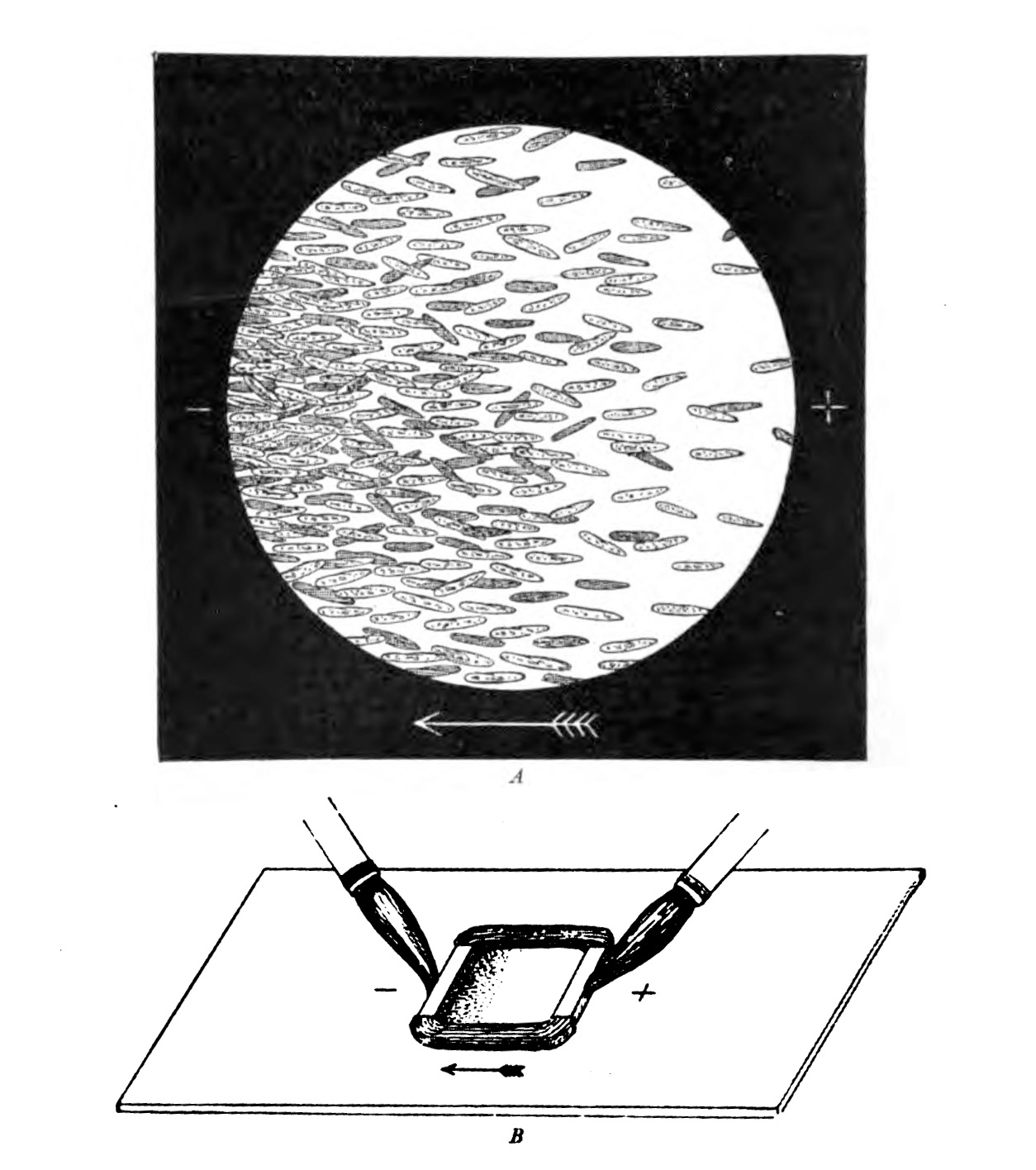
On the finish of the 19th century, the German physiologist Max Verworn watched as a single-celled marine creature was drawn throughout the floor of his slide as if captured by a tractor beam. It had been, in a means: beneath the affect of an electrical subject, it squidged over to the cathode (the pole that pulls optimistic cost). Many different varieties of cells could possibly be coaxed to obey the directional wiles of an electrical subject, a phenomenon generally known as galvanotaxis.
However this was too bizarre for biology, and charlatans already occupied an excessive amount of of the area within the Venn diagram the place electrical energy met drugs. (The affiliation was formalized in 1910 within the Flexner Report, commissioned to enhance the dismal state of American medical colleges, which despatched electrical drugs into exile together with the likes of homeopathy.) Everybody politely forgot about galvanotaxis till the 1970s and ’80s, when the peculiar habits resurfaced. Yeast, fungi, micro organism, you title it—all of them appreciated a cathode. “We had been pulling each sort of cell alongside on petri dishes with an electrical subject,” says Ann Rajnicek of the College of Aberdeen in Scotland, who was among the many first group of researchers who tried to find the mechanism when scientific curiosity reawakened.
Galvanotaxis would have raised few eyebrows if the habits had been confined to neurons. These cells have advanced receptors that sense electrical fields; they’re a basic side of the mechanism the nervous system makes use of to ship its info. Certainly, the rationale neurons are so amenable to electrical manipulation within the first place is that electrical implants hijack a comparatively predictable mechanism. Zap a nerve or a muscle and you’re forcing it to “converse” a language during which it’s already fluent.
Non-excitable cells comparable to these present in pores and skin and bone don’t share these receptors, but it surely retains getting extra apparent that they someway nonetheless sense and reply to electrical fields.
Why? We hold discovering extra causes. Galvanotaxis, for instance, is more and more understood to play an important position in wound therapeutic. In each species studied, damage to the pores and skin produces an immediate, internally generated electrical subject, and there’s overwhelming proof that it guides patch-up cells to the middle of the wound to begin the rebuilding course of. However galvanotaxis will not be the one means these cells are led by electrical energy. Throughout improvement, immature cells appear to sense the electrical properties of their neighbors, which performs a task of their future id—whether or not they grow to be neurons, pores and skin cells, fats cells, or bone cells.
Intriguing as this all was, nobody had a lot luck turning such insights into drugs. Even makes an attempt to go after the lowest-hanging fruit—by exploiting galvanotaxis for novel bandages—had been for a few years at finest hit and miss. “Once we’ve stumble upon wounds which are intractable, resistant, and won’t heal, and we apply an electrical subject, solely 50% or so of the instances truly present any impact,” says Anthony Guiseppi-Elie, a senior fellow with the American Worldwide Institute for Medical Sciences, Engineering, and Innovation.
Nevertheless, previously few years, researchers have discovered methods to make electrical stimulation outdoors the nervous system much less of a coin toss.
That’s right down to regular progress in our understanding of how precisely non-neural cells decide up on electrical fields, which has helped calm anxieties across the mysticism and the Frankenstein associations which have attended organic responses to electrical energy.
The primary massive win got here in 2006, with the identification of particular genes in pores and skin cells that get turned on and off by electrical fields. When pores and skin is injured, the physique’s native electrical subject orients cells towards the middle of the wound, and the physiologist Min Zhao and his colleagues discovered essential signaling pathways which are turned on by this subject and mobilized to maneuver cells towards this pure cathode. He additionally discovered related receptors, and different scientists added to {the catalogue} of adjustments to genes and gene regulatory networks that get switched on and off beneath an electrical subject.
What has grow to be clear since then is that there isn’t any easy mechanism ready on the finish of the rainbow. “There isn’t one single grasp protein, so far as anyone is aware of, that regulates responses [to an electric field],” says Daniel Cohen, a bioengineer at Princeton College. “Each cell sort has a distinct cocktail of stuff protruding of it.”
However current years have introduced excellent news, in each experimental and utilized science. First, the experimental platforms to research gene expression are in the midst of a change. One advance was unveiled final 12 months by Sara Abasi, Guiseppi-Elie, and their colleagues at Texas A&M and the Houston Methodist Analysis Institute: their fastidiously designed analysis platform saved observe of pertinent mobile gene expression profiles and the way they modify beneath electrical fields—particularly, ones tuned to intently mimic what you discover in biology. They discovered proof for the activation of two proteins concerned in tissue progress together with elevated expression of a protein referred to as CD-144, a particular model of what’s generally known as a cadherin. Cadherins are essential bodily constructions that allow cells to stay to one another, appearing like little handshakes between cells. They’re essential to the cells’ skill to behave en masse as an alternative of individually.
The opposite massive enchancment is in instruments that may reveal simply how cells work collectively within the presence of electrical fields.
A unique sort of electroceutical
A serious restrict on previous experiments was that they tended to check the consequences {of electrical} fields both on single cells or on complete animals. Neither is kind of the correct scale to supply helpful insights, explains Cohen: measuring these dynamics in animals is too “messy,” however in single cells, the dynamics are too synthetic to let you know a lot about how cells behave collectively as they heal a wound. That habits emerges solely at related scales, like hen flocks, colleges of fish, or street site visitors. “The mathematics is equivalent to explain a lot of these collective dynamics,” he says.
In 2020, Cohen and his workforce got here up with an answer: an experimental setup that strikes the steadiness between single cell (tells you subsequent to nothing) and animal (tells you too many issues directly). The gadget, referred to as SCHEEPDOG, can reveal what’s going on on the tissue stage, which is the related scale for investigating wound therapeutic.
It makes use of two units of electrodes—a bit the best way you may twiddle the dials on an Etch A Sketch—positioned in a closed bioreactor, which higher approximates how electrical fields function in biology. With this setup, Cohen and his colleagues can exactly tune {the electrical} setting of tens of 1000’s of cells at a time to affect their habits.
Their subsequent “healing-on-a-chip” platform yielded an attention-grabbing discovery: pores and skin cells’ response to an electrical subject relies on their maturity. The much less mature, the better they had been to regulate.
The perpetrator? These cadherins that Abasi and Guiseppi-Elie had additionally noticed altering beneath electrical fields. In mature cells, these little handshakes had grow to be so robust {that a} competing electrical subject, as an alternative of gently guiding the cells, brought on them to tear aside. The immature pores and skin cells adopted the electrical subject’s instructions with out grievance.
After they discovered a technique to dial down the cadherins with an antibody drug, all of the cells synchronized. For Cohen, the lesson was that it’s extra essential to take a look at the system, and the collective dynamics that govern a habits like wound therapeutic, than at what is occurring in any single cell. “That is actually essential as a result of many scientific makes an attempt at utilizing electrical stimulation to speed up wound therapeutic have failed,” says Guiseppi-Elie, and it had by no means grow to be clear why some labored and others some didn’t.
Cohen’s workforce is now working to translate these findings into next-generation bioelectric plasters. They’re removed from alone, and the payoff is greater than pores and skin deep. Numerous work is happening, a few of it open and a few behind closed doorways with patents being intently guarded, says Cohen.
At Stanford, the College of Arizona, and Northwestern, researchers are creating sensible electrical bandages that may be implanted beneath the pores and skin. They’ll additionally monitor the state of the wound in actual time, growing the stimulation if therapeutic is simply too gradual. More difficult, says Rajnicek, are methods to interface with much less accessible areas of the physique. Nevertheless, right here too new instruments are revealing intriguing artistic options.
Electrical fields don’t must immediately change cells’ gene expression to be helpful. There’s one other means their utility could be turned to medical profit. Electrical fields evoke reactive oxygen species (ROS) in organic cells. Usually, these charged molecules are a by-product of a cell’s on a regular basis metabolic actions. Should you induce them purposefully utilizing an exterior DC present, nonetheless, they are often hijacked to do your bidding.
Beginning in 2020, the Swiss bioengineer Martin Fussenegger and a global workforce of collaborators started to publish investigations into this mechanism to energy gene expression. He and his workforce engineered human kidney cells to be hypersensitive to the induced ROSs in portions that ordinary cells couldn’t sense. However when these had been generated by DC electrodes, the kidney cells might sense the minute portions simply tremendous.
Utilizing this instrument, in 2023 they had been capable of create a tiny, wearable insulin manufacturing facility. The designer kidney cells had been created with an artificial promoter—an engineered sequence of DNA that may drive expression of a goal gene—that reacted to these faint induced ROSs by activating a cascade of genetic adjustments that opened a faucet for insulin manufacturing on demand.
Then they packaged this electrogenetic contraption right into a wearable gadget that labored for a month in a residing mouse, which had been engineered to be diabetic (Fussenegger says that “others have proven that implanted designer cells can typically be lively for over a 12 months”). The designer cells within the wearable are saved alive by algae gelatine however are fed by the mouse’s personal vascular system, allowing the change of vitamins and protein. The cells can’t get out, however the insulin they secrete can, seeping straight into the mouse’s bloodstream. Ten seconds a day {of electrical} stimulation delivered by way of needles linked to a few AAA batteries was sufficient to make the implant carry out like a pancreas, returning the mouse’s blood sugar to nondiabetic ranges. Given how straightforward it could be to generalize the mechanism, Fussenegger says, there’s no cause insulin must be the one drug such a tool can generate. He’s fast to emphasize that this wearable gadget may be very a lot within the proof-of-concept stage, however others outdoors the workforce are enthusiastic about its potential. It might present a extra direct electrical different to the answer electroceuticals promised for diabetes.
Escaping neurochauvinism
Earlier than the concerted push round branding electroceuticals, efforts to faucet the peripheral nervous system had been fragmented and didn’t share a lot knowledge. Right now, because of SPARC, which is winding down, data-sharing sources have been centralized. And cash, each direct and oblique, for the electroceuticals challenge has been lavish. Therapies—particularly vagus nerve stimulation—have been the topic of “a gradual enhance in funding and curiosity,” says Imran Eba, a accomplice at GSK’s bioelectronics funding arm Motion Potential Enterprise Capital. Eba estimates that the preliminary GSK seed of $50 million at Motion Potential has grown to about $200 million in belongings beneath administration.
Whether or not you name it bioelectronic drugs or electroceuticals, some researchers want to see the definition tackle a broader remit. “It’s been a particularly neurocentric strategy,” says Daniel Cohen.
Neurostimulation has not but proven success in opposition to most cancers. Different types of electrical stimulation, nonetheless, have proved surprisingly efficient. In a single research on glioblastoma, tumor-treating fields supplied {an electrical} model of chemotherapy: an electrical subject blasts a mind tumor, preferentially killing solely cells whose electrical id marks them as dividing (which most cancers cells do, pathologically—however neurons, being totally differentiated, don’t). A research lately printed in The Lancet Oncology means that these fields might additionally work in lung most cancers to spice up present medication and prolong survival.
All of this factors to extra refined interventions than a zap to a nerve. “The advanced issues that we have to do in drugs will probably be about speaking with the collective decision-making and problem-solving of the cells,” says Michael Levin. He has been working to repurpose already-approved medication to allow them to be used to focus on {the electrical} communication between cells. In a humorous twist, he has taken to calling these medication electroceuticals, which has ruffled some feathers. However he would definitely discover assist from researchers like Cohen. “I might describe electroceuticals way more broadly as something that manipulates mobile electrophysiology,” Cohen says.
Even interventions with the nervous system could possibly be helped by increasing our understanding of the methods nerve cells react to electrical energy past motion potentials. Kim Gokoffski, a professor of scientific ophthalmology on the College of Southern California, is working with galvanotaxis as a doable technique of repairing injury to the optic nerve. In prior experiments that contain regrowing axons—the cables that carry messages out of neurons—these new nerve fibers are likely to miss the goal they’re meant to rejoin. Current approaches “are all pushing the gasoline pedal,” she says, “however nobody is controlling the steering wheel.” So her group makes use of electrical fields to information the regenerating axons into place. In rodent trials, this has labored nicely sufficient to partially restore sight.
And but, Cohen says, “there’s large social stigma round this that’s considerably hampering all the subject.” That stigma has dramatically formed analysis path and funding. For Gokoffski, it has led to difficulties with publishing. She additionally recounts listening to a senior NIH official check with her lab’s work on reconnecting optic nerves as “New Age–y.” It was a nasty shock: “New Age–y has a really unhealthy connotation.”
Nevertheless, there are indicators of extra assist for work outdoors the neurocentric mannequin of bioelectric drugs. The US Protection Division funds initiatives in electrical wound therapeutic (together with Gokoffski’s). Motion Potential’s authentic remit—confined to focusing on peripheral nerves with electrical stimulation—has expanded. “We have now a broader strategy now, the place vitality (in any type, be it electrical, electromagnetic, or acoustic) could be directed to control neuronal or different mobile actions within the physique,” Eba wrote in an e mail. Three of the businesses now of their portfolio concentrate on areas outdoors neurostimulation. “Whereas we don’t have any investments focusing on wound therapeutic or regenerative drugs particularly, there isn’t any express exclusion right here for us,” he says.
This means that the “social stigma” Cohen described round electrical drugs outdoors the nervous system is slowly starting to abate. But when such initiatives are to actually flourish, the sphere must be supported, not simply tolerated—maybe with its personal street map and devoted NIH program. Whether or not or not bioelectric drugs finally ends up following something like the unique electroceuticals street map, SPARC ensured a flourishing analysis group, one that’s in sizzling pursuit of promising alternate options.
Using electrical energy outdoors the nervous system wants a SPARC program of its personal. But when historical past is any information, first it wants a catchy title. It might probably’t be “electroceuticals.” And the researchers ought to positively examine the trademark listings earlier than rolling it out.
Sally Adee is a science and know-how author and the writer of We Are Electrical: Contained in the 200-12 months Hunt for Our Physique’s Bioelectric Code, and What the Future Holds.